You open the mail, or your portal notification pops up, and there it is. Denied.
Maybe it’s treatment after a car crash. Maybe it’s imaging, rehab, follow-up care, home support, or a large hospital bill after a truck wreck. You already have enough on your plate. Pain. Missed work. Calls from adjusters. Family members asking what happens next. Then the insurer sends a letter that sounds final, technical, and cold.
It usually isn’t final.
A denial letter feels personal, but in practice, denials are often part of a system. Claims get rejected for coding issues, “medical necessity” disputes, network arguments, incomplete records, or reasons that don’t hold up once someone pushes back with the right documents. The people who know how to appeal an insurance claim denial treat that first rejection for what it is. A position taken by the insurer, not the last word.
That Sinking Feeling The Day the Denial Letter Arrives
A common initial mistake is assuming the denial means they did something wrong.
Often, they didn’t. They got hurt, sought care, followed doctor instructions, and trusted the insurance process to work. Then a letter arrives filled with claim numbers, explanation codes, and vague phrases that seem designed to wear them down.

That reaction is normal. So is the anger.
What matters next is understanding that denial letters are common, and they’re often challenged successfully. In the US, nearly one in five in-network insurance claims are initially denied, yet less than 1% of these denials are ever appealed. Evidence shows up to 80% of appeals succeed, with 44% overturned on initial internal review and another 27% on external review, according to this review of insurance denial and appeal outcomes.
That changes the frame. A denial is not just bad news. It’s the start of a process that many people could win if they pressed forward.
Practical rule: Don’t treat the denial letter as a verdict. Treat it as the insurer’s opening position.
After a crash, people often need help dealing with multiple insurance problems at once. Medical billing, auto coverage, MedPay issues, lost wages, and liability claims can overlap in ways that aren’t obvious at first. If you’re trying to sort out the broader insurance mess after a collision, this guide on dealing with insurance after a car accident can help you understand how the pieces fit together.
Why the letter feels stronger than it is
Denial letters are written in the insurer’s language, not yours. They sound definitive because they’re supposed to discourage pushback. But the paper itself usually contains the roadmap for challenging the decision.
Read it once for the big picture. Then read it again like evidence.
Look for the reason given, the appeal instructions, the deadline, and any codes or policy terms the insurer relied on. Those details tell you what the company says happened. Your appeal is where you show why that position is wrong, incomplete, or unsupported.
Deconstructing the Denial Your First Clues Are in the Fine Print
Most denial letters look dense on purpose. Strip away the formatting, and they usually answer four basic questions:
- What claim was denied.
- Why the insurer says it was denied.
- How long you have to challenge it.
- Where the appeal has to be sent.
If you miss one of those, you can lose a strong appeal on a technicality.

What to pull from the letter first
Start with a pen or highlighter and mark these items immediately:
- Claim number and policy number. You’ll use both on every communication.
- Date on the denial letter. Deadlines often run from the date of notice.
- Appeal deadline. Appeal deadlines are typically 60 to 180 days according to this step-by-step appeal guide.
- Exact reason for denial. Don’t paraphrase it yet. Quote it in your notes.
- Submission method. Mail, fax, online portal, or a combination.
- Appeals department contact information. Get the direct address, fax, or portal details right.
That deadline is more critical than often understood. A good case can collapse if the appeal arrives late, goes to the wrong address, or doesn’t include the forms the insurer requested.
What common denial reasons usually mean
Insurance companies often use a short label that sounds simple but covers a lot of ground.
Not medically necessary
This doesn’t always mean your treatment was unnecessary. It often means the insurer says the records submitted didn’t justify the care under its standards. In a crash case, that may happen when the records fail to connect symptoms to the collision, don’t describe functional loss clearly, or don’t explain why a given treatment was needed now.
Your response should focus on physician support, clinical records, and the link between the accident and the treatment.
Coding or billing error
This is often the most fixable type of denial. A wrong code, mismatch, duplicate submission, or intake error can trigger a denial even when the treatment itself should be covered. The same appeal guide notes that denial letters often identify coding errors as a stated basis for rejection, and it stresses checking the EOB and provider records closely.
Policy exclusion
This means the insurer claims the policy does not cover the service or circumstance. Sometimes that’s correct. Sometimes the insurer is applying the wrong exclusion, reading the policy too broadly, or ignoring another coverage provision.
For this step, you need the actual policy language, not just the insurer’s summary.
Out of network
In a personal injury setting, this issue can get messy fast. Emergency treatment, referral chains, lack of available in-network specialists, and post-crash care transitions can complicate what sounds like a simple network dispute. If the insurer relies on network status, look carefully at the dates, provider status, referral path, and what the plan required at the time care was delivered.
A quick explainer can help if you need a visual overview before you start sorting the paperwork:
Read the codes, not just the paragraph
The denial code or EOB code can matter as much as the narrative. It tells you which internal rule the insurer used.
Write down every code on the letter and every phrase tied to that code. Then compare it against:
- your bill,
- your provider notes,
- your policy language,
- and any preauthorization or referral records.
The insurer has to tell you why it denied the claim. Your job is to force them to defend that reason with the actual file and actual policy terms.
That shift matters. You’re no longer arguing with a vague “no.” You’re addressing a specific position that can be tested.
Building Your Case How to Gather Undeniable Evidence
An appeal wins when the file becomes hard to ignore.
Many individuals send too little, too late, and in no useful order. They attach a denial letter, maybe a bill, maybe a short note saying the decision is unfair, and hope someone on the other end puts the puzzle together. That rarely works. The insurer won’t build your case for you.
Build it like a lawyer would build a claim file. Organize it. Label it. Make it easy for a reviewer to follow.
Start with the core packet
Every appeal file should include the key documents in one place. If they’re scattered across texts, email chains, provider portals, and paper folders, pull them together first.
A strong packet usually includes:
- The denial letter and EOB. These define what you’re appealing.
- The relevant policy pages. Include the coverage terms, exclusions, appeal rights, and definitions the insurer relied on.
- Medical records tied to the denied care. Office visits, imaging reports, hospital records, therapy notes, discharge instructions, and specialist evaluations.
- Bills and itemized statements. These help match the denied charge to the care provided.
- A timeline of treatment. Date of crash, onset of symptoms, major appointments, referrals, and the denied service.
- Prior communications. Save portal messages, emails, claim notes, and records of calls.
Don’t dump a stack of papers into an envelope. Use a simple index. Number the pages if you can. Put the strongest supporting records near the front.
The document that often changes everything
Most guides stop with “gather your records.” That’s not enough.
Ask for the insurer’s full claim file in writing. This is one of the most useful steps in the entire appeal process, and many claimants never know to do it. The claim file can include the criteria the insurer used, internal notes, reports, correspondence, and the materials reviewed before the denial. A detailed discussion of this tactic notes that policyholders can demand the claim file and that insurers are legally required to provide it within 30 days, as explained in this article on requesting and using the insurer’s claim file.
That request matters because you can’t effectively challenge hidden reasoning if you never see it.
What the claim file can reveal
When the file arrives, look for three things.
The actual standard used
Insurers often summarize the reason for denial in broad language. The file may show the narrower internal standard or review criteria behind that summary. Sometimes the denial turns on a definition or utilization rule that never appeared clearly in the letter.
Missing or incorrect facts
Internal notes may rely on a mistaken diagnosis history, the wrong date of injury, incomplete records, or an assumption that treatment was unrelated to the crash. If the file reveals a factual error, your appeal should call it out directly and attach proof.
Gaps in review
Sometimes the reviewer never had the best records. Sometimes there’s no sign the insurer considered the treating doctor’s explanation. Sometimes adjuster notes show a rushed or incomplete process. Those are not small issues. They’re the kind of issues that can frame the entire appeal.
File-building rule: Don’t only prove you deserve coverage. Show exactly where the insurer’s reasoning breaks down.
Get your doctors involved the right way
A short, generic doctor note often doesn’t move the needle. You want a targeted letter of medical necessity that addresses the reason for denial.
Ask the provider to cover:
- the diagnosis,
- how the accident caused or worsened the condition,
- why the denied treatment was necessary,
- what functional problems you had without it,
- and why lower-level or alternative care would not have been adequate.
For personal injury cases, the best letters connect medicine to daily life. A strong letter explains not only the diagnosis, but what the patient couldn’t do, what risks existed without treatment, and how the requested care fit the actual post-crash condition.
If you’re still early in the process of organizing the injury side of the case, this primer on filing a personal injury claim is a helpful companion to the appeal work.
Use presentation as a strategy
Presentation isn’t cosmetic. It affects whether your evidence gets read and understood.
A solid appeal packet often includes:
- A cover page listing the claim number, policy number, and denial date.
- A table of enclosed documents.
- The appeal letter.
- The denial letter and EOB.
- Medical necessity support.
- Medical records in date order.
- Billing records.
- Policy excerpts.
- Any claim file excerpts that undermine the denial.
Send it the way the insurer requires. If mail is permitted, use certified mail with return receipt. If the insurer requires a portal, upload a complete PDF and save the confirmation. Keep a duplicate copy of everything exactly as sent.
That level of organization does two things. It helps the reviewer follow your case, and it signals that you’re documenting the process carefully. Insurers pay attention when they see that.
Drafting a Powerful Appeal Letter That Gets Results
The appeal letter should sound calm, specific, and difficult to brush aside.
At this point, many strong claims go sideways. People write angry letters. They tell the insurer the denial is outrageous, heartless, or absurd. They describe how stressed they are, how unfair life feels, and how much pain they’re in. All of that may be true. It usually isn’t the most effective way to persuade a reviewer.
Write for the file, not for catharsis.
What the letter should include
A good appeal letter has a simple structure.
Opening
Identify the claim, state that you are appealing the denial, and name the denied service or bill. Keep it direct.
Example:
I am appealing the denial of coverage for treatment related to injuries sustained in a motor vehicle collision. The denial letter dated [date] states that the claim was denied for lack of medical necessity.
Middle section
Address the denial reason point by point. Quote the insurer’s stated basis. Then answer it with documents.
Use phrasing like:
- “The denial states…”
- “The medical records attached at Tab 4 show…”
- “The treating provider’s letter explains…”
- “The policy language at page… provides…”
That format forces the reviewer to deal with specifics.
Weak phrasing versus strong phrasing
| Weak approach | Strong approach |
|---|---|
| “You denied this unfairly and I need help.” | “The denial states the treatment was not medically necessary. The attached treating physician letter explains the diagnosis, post-collision symptoms, and why this treatment was required.” |
| “My doctor says I need it.” | “The attached provider statement ties the requested care to the crash-related condition and explains why the requested treatment was appropriate under the policy terms.” |
| “Please reconsider.” | “I request that the insurer reverse the denial and issue coverage for the submitted claim based on the attached medical records, billing records, and policy language.” |
Tone wins more often than volume
The strongest letters are firm, not theatrical.
If the insurer made an obvious mistake, say so plainly. If the denial misstates the records, point to the exact page that fixes the error. If the policy supports coverage, cite that section. Precision has more force than indignation.
A useful closing might read like this:
Based on the enclosed records, the denial should be reversed. Please confirm receipt of this appeal and provide written notice of the insurer’s decision within the applicable review period.
That’s clean and effective. It preserves your credibility and creates a paper trail.
What not to do
Avoid these common missteps:
- Don’t ramble. A long, unfocused narrative weakens strong evidence.
- Don’t exaggerate. If a record says “improving,” don’t claim it says “permanently disabled.”
- Don’t rely on phone calls alone. Put the argument in writing.
- Don’t ignore the policy language. The insurer will not.
If you want to know how to appeal an insurance claim denial effectively, this is the heart of it. Match every denial reason to a document, a fact, or a policy provision. Make the reviewer choose between your organized record and the insurer’s thinner explanation.
The Appeal Journey Navigating Internal and External Reviews
A lot of people think there is one appeal. In practice, there can be layers.
The first level is usually an internal appeal. That means the insurer reviews its own denial. If that fails, there may be another internal level depending on the policy. After internal appeals are exhausted, the most important shift happens. You can seek an external review by an independent reviewer.
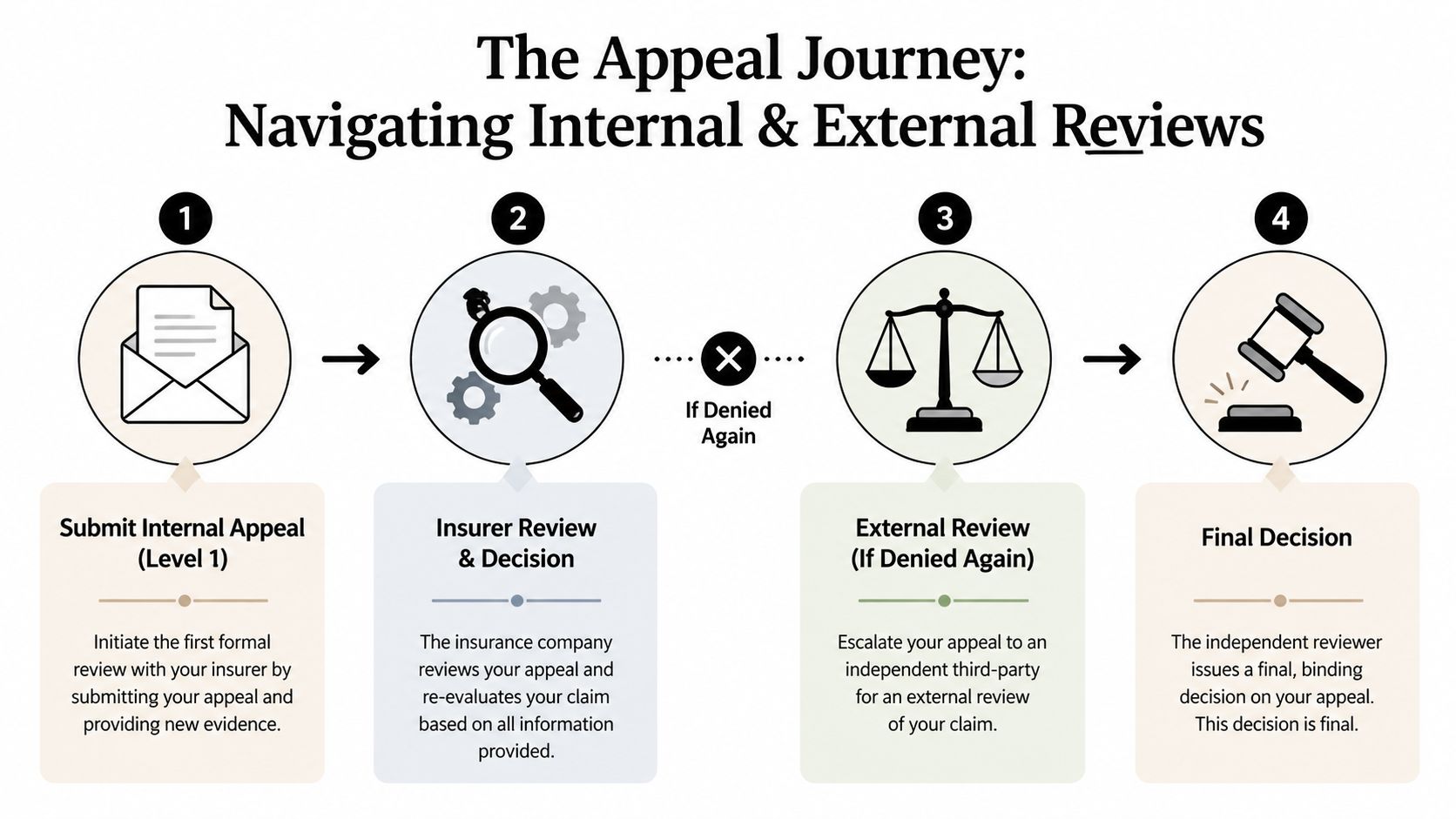
Internal review is not the end of the road
An internal appeal matters because it preserves your position and builds the record. It also gives you the chance to correct missing documents, add a stronger medical necessity letter, and challenge the insurer’s stated basis before an outside reviewer sees the case.
Don’t expect the insurer to volunteer what’s missing. You need to assume responsibility for a full submission.
A practical way to think about internal review is this:
- Level 1 is where you present the corrected and organized case.
- A second internal review, if available, is where you fix what the first review still ignored.
- External review is where the argument gets removed from the insurer’s own financial control.
Why external review is such a powerful step
Once internal appeals are exhausted, you can request external review. Impartial experts overturn approximately 40% to 60% of denials because they are not biased by the insurer's financial interests. For high-value claims in motor vehicle accidents, a strong letter of medical necessity is a factor in 85% of successful external reviews, according to this guide on internal and external appeals.
That’s why persistence matters. The same denial that survived an internal review may not survive outside scrutiny.
When the insurer controls the review, you are asking it to admit it was wrong. In an external review, you are asking an independent evaluator to judge the record.
That’s a very different posture.
How to move through the levels without losing ground
Keep one master file
Don’t create a fresh, inconsistent appeal at each stage. Use a master file with your core records, then add new evidence and a short update memo as the process continues.
Track every deadline and confirmation
Appeals are lost on procedure more often than people think. Save portal confirmations. Keep mailing receipts. Log every call with the date, time, name, and what was said.
Add, don’t just repeat
If the first internal appeal failed, don’t send the exact same packet again unless the denial clearly ignored materials already submitted. Add something useful. A clearer doctor letter. Claim file excerpts. Better policy citations. A short explanation of what the prior reviewer missed.
Typical response windows
Under the same step-by-step framework discussed earlier, insurers must respond within strict timelines: 72 hours for urgent care appeals, 30 days for pre-treatment denials, or 60 days for post-treatment under NAIC guidelines, as summarized in the previously linked appeal guidance. Those timelines give you a way to measure whether the insurer is moving the file appropriately.
If the case involves urgent post-crash care, ask immediately whether expedited review is available.
Special Rules for Colorado Motor Vehicle and Trucking Accidents
A denial after a Colorado crash often looks like a routine paperwork problem. It usually is not.
Auto claims, health coverage, MedPay, hospital liens, and liability positions can start to overlap fast after a serious wreck. In trucking cases, the file may also involve commercial carrier records, federal safety issues, and catastrophic injury proof that a standard appeal packet never addresses. If you treat that denial like a generic health insurance dispute, you can miss arguments that matter.

Urgent injury claims in Colorado
With brain injuries, spinal trauma, or post-surgical care after a wreck, delay can change the medical outcome. Ask for expedited review in writing if the denied treatment is time-sensitive. Do not rely on a phone call alone.
In Colorado crash cases, I want the request to say exactly what goes wrong if care is delayed. Missed rehab window. Loss of specialist access. Risk of permanent worsening. Attach a treating provider statement that says the same thing in clear terms. Vague urgency language gives the insurer room to stall.
It also helps to ask for the insurer’s complete claim file at the same time, including nurse notes, peer review reports, internal guidelines, and any document the reviewer used to support the denial. That request often exposes shortcuts, missing records, or a reviewer who focused on cost instead of medical need.
Trucking cases require a different build
Truck wreck appeals often involve bigger injuries and more complicated records. They also raise issues that do not show up in an ordinary passenger-car claim.
For example, the insurer may minimize treatment by calling the condition degenerative or unrelated to the crash, even when the mechanism of injury says otherwise. In a trucking case, the force of impact, vehicle weight, scene evidence, ECM data, hours-of-service issues, and post-crash investigation materials can all help explain why the injuries are serious and why the treatment is reasonable. Those facts do not replace medical proof, but they can strengthen causation.
I also look closely at whether the denial ignores commercial-driver or carrier records already in circulation. If those materials support a high-energy collision and the medical reviewer never addressed them, that is worth pointing out directly in the appeal.
What Colorado crash victims should do differently
A strong Colorado motor vehicle or trucking appeal usually needs more than office notes and bills. Send a tighter record.
Focus on:
- Crash-specific causation proof. ER records, imaging, specialist reports, and provider letters should connect the symptoms and treatment to the collision in plain language.
- A clean timeline. Show what happened before the wreck, what changed after it, and why any treatment gap has a real explanation.
- Functional loss evidence. Work restrictions, driving limits, missed job duties, memory problems, sleep disruption, and household limitations can make the medical need harder to dismiss.
- The insurer’s own file. Request adjuster notes, utilization review materials, medical reviews, and internal claim handling documents so you can answer the denial on its actual terms.
- Commercial vehicle context. In truck cases, include crash reports, preservation letters, and other records that show this was not a minor-impact event.
A serious Colorado wreck appeal is part of the broader injury case. The insurer is evaluating not just bills, but the full scope of harm and what it may have to pay later.
If the denial involves a truck crash, severe injuries, or multiple layers of coverage, it may be time to get legal help before you lock in a weak record. This guide on when to hire a personal injury attorney for your case explains the warning signs.
Knowing When to Tag in a Professional Your Red Flags List
Some appeals are manageable on your own. Some aren’t.
You should consider getting legal help when the denial stops being a paperwork problem and starts looking like a strategy. If the insurer keeps shifting reasons, delays responses, ignores records you submitted, or misstates what the policy says, that’s a warning sign.
Other red flags are straightforward:
- Catastrophic injury. Traumatic brain injury, spinal trauma, or long-term disability.
- Large medical exposure. Bills are growing and treatment is ongoing.
- Truck wreck involvement. Multiple policies, serious injuries, and federal issues can complicate the appeal.
- External review denial despite strong records. At that point, the next move may require a broader legal strategy.
- You can’t keep up. If your health, family responsibilities, or work demands make the process unmanageable, that matters.
If you’re weighing whether it’s time to bring in counsel, this guide on when to hire a personal injury attorney for your case lays out the decision points clearly.
Frequently Asked Questions About Insurance Appeals
The denial letter is on the table, bills are still coming in, and every deadline suddenly feels dangerous. These are the questions clients ask when they need clear next steps, not insurance jargon.
| Question | Answer |
|---|---|
| Can I appeal if the insurer says the treatment wasn’t medically necessary? | Yes. That is a common denial, and it can often be challenged with the right record. Build the appeal around a detailed medical necessity letter, treatment notes, and a clear explanation of how the care relates to the crash injuries. |
| What if the denial was caused by a billing or coding issue? | Start with the provider’s billing office right away. Ask for a coding review, corrected claim forms if needed, and a copy of what was resubmitted. Then keep that paper trail and send the corrected material with your appeal if the insurer still refuses payment. |
| Should I call the insurer before I send the appeal? | Yes, but treat the call as information gathering only. Confirm the deadline, mailing address, fax number, portal instructions, and whether the insurer requires a specific form. Then send the appeal in writing and keep proof that it was delivered. |
| What is the claim file and why should I request it? | The claim file can show the insurer’s internal notes, review criteria, adjuster comments, and the documents used to support the denial. That matters because you can see what the reviewer relied on, what was ignored, and whether the stated reason changed over time. In vehicle and trucking cases, I often want that file early because it can expose shortcuts in how the insurer evaluated causation or medical need. |
| Can my doctor help with the appeal? | Yes. A treating doctor can address the insurer’s weak points directly, especially on medical necessity, accident causation, future treatment, and functional limitations. A short, specific letter usually carries more weight than a generic chart note. |
| What if I miss the appeal deadline? | Act the same day you realize it. Ask the insurer, in writing, whether any extension, reopening process, or alternate review is available, and explain why the deadline was missed if there is a legitimate reason. Late appeals are harder, but silence is worse. |
| Is an external review worth the effort? | Often, yes. An outside reviewer is not defending the insurer’s earlier decision, and that change can matter. If the internal denial ignored strong records, misstated the policy, or brushed past a treating doctor’s opinion, external review may give the file a fairer look. |
| Are there special appeal issues after a Colorado car crash or truck wreck? | Yes. Colorado injury claims often involve overlapping sources of payment, including Med Pay, health coverage, and liability issues tied to the crash. Trucking cases can add another layer because serious injuries, multiple insurers, and larger treatment plans tend to trigger closer scrutiny. In these claims, deadlines, claim file requests, and precise medical support matter even more. |
| Will appealing make the insurer retaliate against me? | A proper appeal is part of the process, and you have every right to file one. The smarter concern is that the insurer will examine your submission closely, so keep it accurate, organized, and consistent with the medical record. Sloppy appeals create openings the insurer will use. |
| What should I do while the appeal is pending? | Keep treating as your doctors recommend. Save every new bill, explanation of benefits, and treatment record. If a provider is sending accounts to collections, ask whether the balance can be marked as disputed while the appeal is under review. |
If you’re dealing with a denied claim after a car crash or truck wreck, Nares Law Group LLC helps injured people in Colorado fight insurance problems with clarity, urgency, and trial-tested strategy. If the denial is threatening your access to care, your finances, or the value of your injury case, reach out for a free consultation.